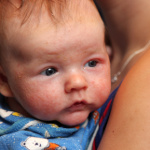
Understanding and Treating Eczema in Babies, Toddlers & Older Children
Eczema (or atopic dermatitis) in children can start as early as two months of age. It’s a very common condition, affecting approximately 10% of infants and children. Here are tips about understanding and treating eczema.
Common Scenarios
Your 13-month-old has been off of formula for a month now and enjoys drinking milk out of her sippy cup. You’ve noticed a red, raised rash scattered in different places around her body. She occasionally scratches it, which seems to make it even worse.
Your 4-month-old has had a red, irritated rash on his face for the past two months. Everyone has told you it’s just baby acne. You now start to see the rash breaking out on his arms, legs, and body. It seems to be getting worse. He is exclusively breastfed.
Your 4-year-old has always had dry skin, but it never seemed to bother him. Lately, however, he has developed dry, scaly patches on his arms, legs, and face.
These are all common scenarios that are typical of eczema.
What is eczema?
Eczema is a skin condition that has two distinct components:
- Dry, easily irritated skin – children with this type of eczema have a genetic tendency toward dry skin. Moisture is very important for our skin. It helps skin stay healthy, prevents irritation, and speeds up healing. Moisture essentially helps our skin function better. With eczema, the skin does not retain moisture very well, thus giving it a dry, slightly rough texture and making it prone to irritation. To further complicate matters, this dry, irritated skin is itchy, causing children to scratch frequently. This further irritates and damages the skin, which leads to worse itching and scratching, and so on.
- Allergies – children with this condition also have some underlying allergies that are manifested in the skin. When exposed to these allergens, the skin over-reacts and breaks out in a rash. The already dry and slightly irritated skin is less able to handle this allergic rash and less able to heal itself quickly.
Thus, children with eczema have an ongoing battle on two fronts – trying to retain moisture in the skin and prevent irritation and itching, and limiting exposure to allergens and skin irritants. This is a battle we plan to help you and your child win against eczema!
Now that we know what causes eczema in babies and toddlers, let’s take a closer look at what symptoms to look for.
What does eczema look like in children?
- Dry skin – your child will have slightly dry skin with a rough texture. You may be able to see and feel tiny white bumps as you run your fingers across the skin.
- Dry patches – you may see scattered, scaly, dry, white patches anywhere on the body.
- Flare-ups – from time to time you will see some areas of the skin become more irritated and flare up due to eczema. These will look like raised, red, slightly oozing patches. Flare-ups generally occur near skin creases – most commonly the inside of the elbows and behind the knees, but also in the neck, wrists and hands, and feet. An eczema rash can also occur on the trunk. One unique aspect of eczema is that it usually does not affect the diaper area.
What causes infant and toddler eczema?
As stated above, eczema is a mixture of dry skin and allergies. The cause is mainly genetic – an inborn tendency toward dry skin and allergies. There is no way to change these genetics. The important issue is not what causes eczema in the first place, but what allergens and skin irritants your child is exposed to that are triggering the flare-ups.
Treating Eczema
There are 5 main aspects of preventing and treating eczema in children:
Avoid dry skin
Moisturize, moisturize, moisturize! This is the single most important step in treating eczema and minimizing your child’s eczema. Do not underestimate this – this is a vital part of toddler and baby eczema treatment. This needs to be part of your daily routine with your child:
- Luke-warm baths – hot water can dry the skin. Let your child play and soak in the bath. Do not let him soak in soapy water. It used to be felt that frequent bathing made eczema worse. Now we know that luke-warm baths allow water to soak into the skin.
- Towel off gently by patting the skin. Do not rub dry.
- Do not use plain soap – soap dries the skin, even liquid baby soap.
- Use a moisturizing soap with no perfume – unscented Dove works very well. Cetaphil is a cleanser that is also soap-free and good for eczema.
- Daily moisturizing lotion – this is very important. Two to four times a day, apply a moisturizing lotion or cream to the whole body, especially the affected areas. Some good brands include Aquaphor, Eucerin, or Keri lotion. One good time to apply this is right after the bath – it locks in the moisture.
Avoid skin irritants
This is the second most important aspect of eczema prevention.
- Cotton clothing is best. Avoid wool and synthetic materials; they can be more abrasive and irritating to the skin.
- Use cotton sheets and soft, cotton blankets.
- Wash new clothes before wearing them – this will get out any chemicals from the manufacturing process.
- Do not use any perfumed or scented lotions.
- Do not use bubble bath.
- Laundry detergents – use a mild, dye-free detergent such as Dreft, Ivory Snow or All Clear. Liquid detergents rinse out better.
- Double rinse the wash to get out all the detergent.
- Shower or bath after your child plays in the grass or engages in sports that make him sweaty.
- Maintain humidity of 25-40 percent in your home. Buy a humidity gauge. During the dry winter months, use a humidifier in your home. During the humid summer months, the air conditioning can keep the humidity stable.
- Suntan lotion – use one that doesn’t irritate your child’s skin. PABA free is better.
Avoid allergic triggers
- Food allergies – if your child has any food allergies, then they will play a major role in causing eczema. The problem is, you may not know if your child has any food allergies, and if he does, which foods is he allergic to? Thankfully, there are six common foods that make up nearly 90 percent of possible allergic foods. These are milk, egg, soy, peanuts, fish, and wheat. Eliminate all six foods for 2 to 3 weeks. If you see a dramatic reduction in eczema flare-ups, then re-introduce each food one at a time to determine which is causing the allergy.
- Environmental allergies – these include dust, mold, pets, and seasonal outdoor allergies such as pollens. These environmental allergies are more likely to cause nasal allergies and asthma rather than eczema. However, they can contribute to eczema. Identifying and preventing these allergies is a very complicated process.
Control the itching
This is a major problem for children with eczema. They are in a continuous cycle of itching and scratching. The dry, irritated skin itches, so your child scratches. The scratching further irritates the skin, which causes the eczema rash to flare up. This itches even more and your child scratches even more. If you can keep the skin moisturized, decrease the rash, and prevent itching and scratching, then you can avoid this endless cycle.
- Keep fingernails cut short and very clean – when your child scratches, the bacteria that live under his nails and on his skin get pushed deeper into the rash. This can lead to a skin infection. Shorter nails also will lessen the trauma to the skin.
- Wear long sleeves and pants, weather permitting – this keeps his skin covered so your child is unable to scratch as much.
- Medications to reduce itching – oral antihistamines are a very effective way to control the itching caused by eczema. There are two types:
- Over-the-counter – Benadryl (diphenhydramine) is the standard for itching. Its only drawback is that it causes drowsiness in many people. At nighttime, this can be an advantage since it will help your child sleep through the itching. But during the day, it can interfere will his daily functioning.
- Non-sedating prescriptions – Zyrtec, Claritin, and Allegra and the three most commonly used. Zyrtec is currently approved for down to age 2 years. The other two are not – so should not be used for infant or toddler eczema treatment. These have two benefits: they are long-acting and last 12 hours, and for most people, they do not cause drowsiness. Thus they are very convenient for use during the day.
- You can alternate between these two. Use Benadryl at night, and a prescription during the day.
- When to use these medications – do not just automatically give these to your child every day. When the eczema is under control, the rash is mild, and your child has little or no itching, then give your child a break from the medication. But do not be afraid to use it during flare-ups and for periods of moderate to severe itching. You need to break the itching and scratching cycle before the rash worsens. You can safely use these medications daily for several weeks.
Topical steroid cortisone cream
Although this is a medication to help control itching as in the section above, it deserves its own special section. These creams have long been the gold standard. It helps in treating eczema by minimizing the rash and itching. They vary in strength from the extremely mild over-the-counter hydrocortisone cream, to mild, medium, strong, and very strong prescription creams. Follow the instructions below for treating eczema with creams.
- Preventative treatment – if your child’s eczema is usually well controlled, with very little itching and rash, then you do not need to use cortisone cream for prevention. However, if the eczema is moderate to severe and your child continuously has rash and itching despite all possible measures to minimize it, then you can use this cream on a daily basis to try to improve the condition. Use the mildest form of infant or toddler eczema cream that seems to work for your child.
- Mild rash – this consists of a few areas of raised, red rash slightly worse than your child’s baseline rash. Treat this with the over-the-counter 1 percent hydrocortisone cream (do not bother with the 0.5 percent – you might as well not use anything if you use this). It will say extra-strength, but it is really very mild. Use the cream twice a day until the rash subsides. Ask your doctor for a mild prescription cortisone cream if the OTC one doesn’t work.
- Moderate rash – again, what is considered moderate is based upon your child’s baseline rash. These areas are often more red and inflamed, may have some oozing from the rash, and may bleed slightly from scratching. The itching will be worse than usual. Treating eczema in these areas with a mild prescription cortisone cream. You can also ask your doctor for a medium strength eczema cream if the mild one doesn’t work.
- Severe rash – these areas will be very red and irritated, will ooze, and bleed. These areas will be larger and more widespread than usual. Itching and burning will be troublesome. Treat this with a medium strength prescription cortisone cream. Your doctor may prescribe a strong cream to be used very sparingly for severe areas that don’t improve with a medium strength cream.
- How long to use eczema cream – only use the prescription cream until the rash subsides. You don’t have to keep using the same strength cream until the rash is totally gone. If you have been treating eczema and you see the rash is somewhat better, then step down to a weaker cream. Use that one until the rash is back to baseline. It is safe to use mild prescription creams for a few weeks.
- Helpful tips – When treating eczema after a bath, apply the cream to the slightly damp skin. Apply the steroid cream before applying the moisturizer.
- Side effects of steroid creams. There are two types of side effects:
- Local side effects in the skin – include thinning of the skin, stretch marks, and infections. Different parts of the body are more susceptible to side effects in the skin. These areas include the face, armpits, and genital areas. It is generally safe to use the mildest creams on these areas for a few weeks, and use the mild to moderate creams for several days, but it is better not to use the strong creams on these areas at all.
- Internal side effects – a very small percentage of the steroid is absorbed through the skin into the bloodstream. If enough is absorbed, it can affect certain hormone levels which in very rare cases can cause a reduced growth rate. Be aware that this only happens with the overuse of the strong steroid creams. The stronger the cream and the longer it is used, the more chance of side effects. Over the counter cream has virtually zero chance of side effects, and so do the mildest prescription creams. The moderate strength creams have a slight chance of side effects. The strong creams have some chance of side effects, especially the longer they are used. The very strongest creams should not be used to treat eczema in children.
- Preventative treatment – if your child’s eczema is usually well controlled, with very little itching and rash, then you do not need to use cortisone cream for prevention. However, if the eczema is moderate to severe and your child continuously has rash and itching despite all possible measures to minimize it, then you can use this cream on a daily basis to try to improve the condition. Use the mildest form of infant or toddler eczema cream that seems to work for your child.
“Soak and Seal”
This is a technique we use in our medical practice: because eczema is basically dry skin, apply a light layer of water over eczema, then cover with the lubricant, which then seals the area and allows the water to soak in.
Skin infections
Be aware that children with eczema are more susceptible to bacterial skin infections, especially in areas where the rash is the worst. This infection is called impetigo. Signs that this is occurring are increased redness of the skin around the rash and a honey-colored fluid oozing from the rash or forming a crust over the rash. This is not an emergency and is not a reason to page your doctor after hours. It can wait until the next day to be seen by the doctor.
New innovations in the treatment of eczema in children
Tacrolimus ointment – this is an investigational ointment currently being tested in the U.S. for the treatment of eczema. It suppresses the part of the immune system that is responsible for the eczema rash and itching. This ointment is showing great promise, and will hopefully be available soon. It appears to be just as effective as steroid creams but does not have many of the side effects that the steroids have.
Will my child ever outgrow eczema?
Yes. For most children, eczema improves during childhood. Your child may always have a very slight problem with dry skin and occasional mild rash, but the vast majority of children grow up with very little inconvenience from this condition.
The best foods for healthy skin are:
- Omega-3 fatty acids, such as flax seeds or flax-seed oil, salmon and tuna fish.
- The antioxidants vitamin C and vitamin E act like nature’s own protection.
- Lots of fluids, preferably water, to help keep your baby’s skin well hydrated.
Dr. Sears, or Dr. Bill as his “little patients” call him, has been advising busy parents on how to raise healthier families for over 40 years. He received his medical training at Harvard Medical School’s Children’s Hospital in Boston and The Hospital for Sick Children in Toronto, the world’s largest children’s hospital, where he was associate ward chief of the newborn intensive care unit before serving as the chief of pediatrics at Toronto Western Hospital, a teaching hospital of the University of Toronto. He has served as a professor of pediatrics at the University of Toronto, University of South Carolina, University of Southern California School of Medicine, and University of California: Irvine. As a father of 8 children, he coached Little League sports for 20 years, and together with his wife Martha has written more than 40 best-selling books and countless articles on nutrition, parenting, and healthy aging. He serves as a health consultant for magazines, TV, radio and other media, and his AskDrSears.com website is one of the most popular health and parenting sites. Dr. Sears has appeared on over 100 television programs, including 20/20, Good Morning America, Oprah, Today, The View, and Dr. Phil, and was featured on the cover of TIME Magazine in May 2012. He is noted for his science-made-simple-and-fun approach to family health.